|
Adhesiolysis for small bowel obstruction and cholecystectomy was performed uneventfully, and there were no issues with pacing. Before surgery, the pacing mode was changed to DOO (asynchronous atrial and ventricular pacing), 70 beats/min, since the patient was pacing dependent. Although the pacemaker had capture management, it had not been enabled. The battery, lead impedances, and sensing amplitudes were acceptable. The ventricular pacing threshold was 1.5 V with 0.4-millisecond duration and the ventricular pacing output was 2.5 V with 0.4-ms duration. The patient’s underlying rhythm was complete atrioventricular block with a very slow ventricular escape rhythm. The pacemaker was interrogated immediately after anesthesia induction by a clinical engineer, which showed that the pacemaker was programmed to the DDD mode with a lower rate limit of 70 beats/min and an upper rate limit of 120 beats/min. Anesthesia was maintained with sevoflurane and remifentanil. The blue arrowhead indicates the ventricular pacing spikes with ventricular capture.Īnesthesia was induced with remifentanil and propofol, and muscle relaxation was achieved with rocuronium. The red arrow indicates the atrial pacing spikes with atrial capture. It demonstrates dual-chamber atrial and ventricular pacing and capture at 70 beats/min. Laboratory data on admission showed a hematocrit of 32.5% but were otherwise unremarkable.Ī 12-lead electrocardiogram recorded when the patient was admitted to the emergency department. An electrocardiogram demonstrated dual-chamber atrial and ventricular pacing and capture at 70 beats/min (Figure (Figure2). Abdominal examination showed tenderness in the right upper quadrant. On examination, he was in moderate distress with a blood pressure of 176/73 mm Hg. 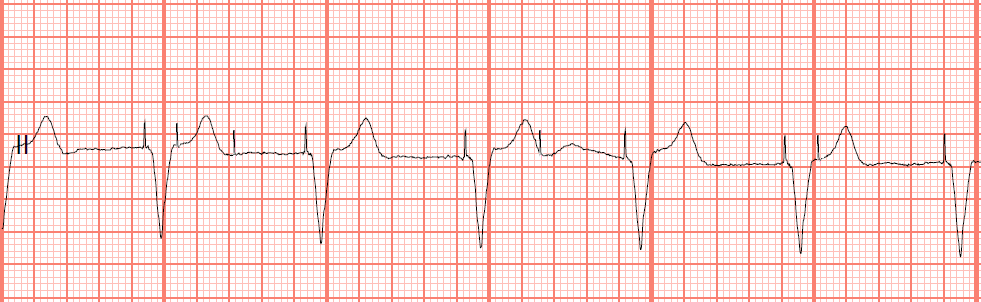
Medications included glargine and vildagliptin. His history included a previous gastrectomy for gastroduodenal ulcer and type 2 diabetes mellitus. Two months before presentation, the pulse generator was upgraded to a Medtronic Advisa (MRI A3DR01, Medtronic Japan) due to battery depletion and was programmed to the DDD (dual chamber pacing and sensing, dual response to sensing) mode with a lower rate limit of 70 beats/min. However, no apparent cause of failure to capture was identified. A cardiologist assessed the patient, and the device (Medtronic EnPulse, E2DR31, Medtronic Japan, Tokyo, Japan) was interrogated. Of note, 5 months before presentation, he had transient loss of pacing capture (Figure (Figure1) 1) during an intensive care unit (ICU) stay for the treatment of septic cholangitis. He had undergone pacemaker implantation 17 years ago for advanced atrioventricular block. Written informed consent has been obtained from the patient for this publication and this article adheres to the applicable Enhancing the QUAlity and Transparency Of health Research (EQUATOR) guideline.Ī 78-year-old man with an acute strangulated small bowel obstruction presented for urgent laparotomy. We describe a patient with a pacemaker who developed sudden cardiac arrest due to pacemaker capture failure shortly after laparotomy and ultrasound-guided rectus sheath block. 5, 6 Therefore, patients with pacemakers are at risk of capture failure during surgery and anesthesia. Known causes include myocardial ischemia, 4 acid-base disturbances, electrolyte imbalance, 5 and antiarrhythmic drugs. 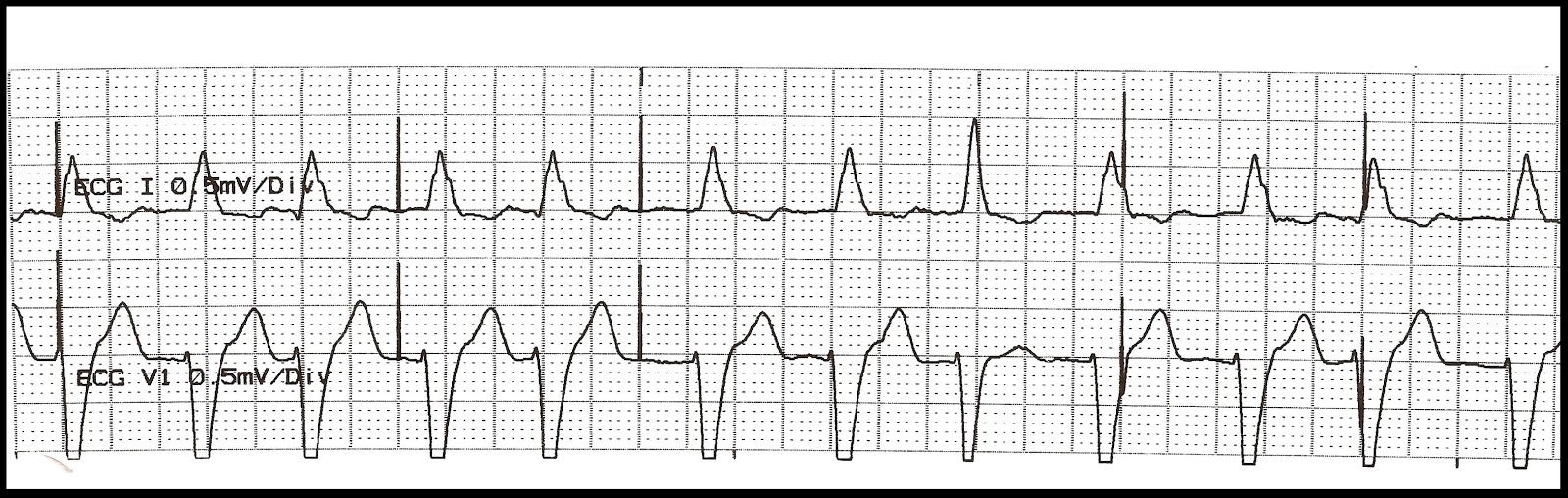 
Failure to capture is an important etiology of pacemaker malfunction. However, perioperative pacemaker malfunction can occur in the absence of EMI. As long as routine preanesthetic device evaluation and appropriate reprogramming are performed, these risks are minimized. Since electrical equipment, such as electrosurgery and other devices that emit radiofrequency signals, can cause electromagnetic interference (EMI), 2, 3 serious complications due to CIED malfunction may occur in the perioperative period. As the prevalence of cardiac pacemaker insertions increases, 1 anesthesiologists are expected to manage more patients with a cardiovascular implantable electronic device (CIED) undergoing anesthesia and surgery.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
